Cancer affecting the breast is detected by appropriate
investigations some of which are listed below:
Breast Imaging
Mammogram
This is an x-ray of the breast. It is able to detect masses, changes
in breast density and depositions of calcium within the ducts of the breast. It is more
effective in the elderly and of limited use in younger ladies as their breasts are more
dense.
Deposition of calcium in the breast tissue is often the earliest
indication of an abnormality in the breast.
More about Mammography
Example
of Mammographic Abnormalities
Example
of Cancer
Ultrasound of the breast
This examination is useful in younger women, where the mammograms are of limited use. It is
able to differentiate between a solid and a cystic structure. Moreover it can often detail
the outline of the breast lump and provide important information.
Pictures of Ultrasound of the breast
MRI of the breast.
MRI is being used for the diagnosis of breast conditions, however its overall significance
in the management of breast diseases is still under evaluation.
Pathological assessment of breast tissue.
The only definite way of diagnosing cancer is by
obtaining proof of its existence in the tissues of the breast. This can be achieved by the
following ways.
Fine Needle Aspiration Cytology (FNAC).
In this method a small needle is inserted in to the mass felt in the
breast and a few cells are aspirated and then spread out on a glass slide. The pathologist
looks at these cells and gives a diagnosis.
Pictures of FNAC being done and Cancer Cells
More about FNAC
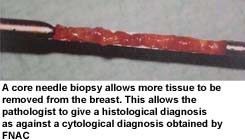
Core needle biopsy.
The principle is the same as the FNAC. However, instead of a few cells
a core of tissue is extracted from the breast. A larger bore needle is used for in this
technique and hence a local aneasthetic agent is used to numb the area prior to inserting
the needle.
Both the above tests can be easily performed in the consulting room.
Open biopsy
In this technique, the mass or abnormal area in the breast is removed
and sent to the pathologist for examination. This requires a cut to be made on the breast
and is done under local or general anaesthesia. More about open
biopsy
Needle-localisation excision biopsy
This method is used for diagnosing tumours which are too small to be
felt by the doctor but are seen on mammogram.
It involves the placement of a fine needle in the breast guided by mammograms. The surgeon then removes
the necessary area around the needle (guided by it) and submits it for examination. |
